
Lifebox: An Organization with its Finger on the Pulse of Surgical Safety
It’s a simple piece of equipment that can save your life in surgery.
Nonprofit organization Lifebox, working to make it available around the world with past support from SNF, has delivered more than 20,000 of them so far.
Surgery is proverbially complex, but when it goes wrong, the causes can be remarkably simple.
In answer, a deceptively simple yet amazingly effective safeguard has gained currency in recent years. The World Health Organization’s (WHO) 19-point Surgical Safety Checklist, first introduced in 2008, is designed to set a minimum global standard for safe surgery, broken down into straightforward, sequential steps.
The aim is not to introduce any steps skilled surgical teams don’t know to do, but rather to facilitate communication and provide a matrix for orderly intentionality in a high-stakes environment.
“Has the patient confirmed his/her identity, site, procedure, and consent?” the checklist begins. “Is the site marked?” it continues.
The low-tech checklist can serve as a remarkably effective safety tool, reducing complications and death from surgery by more than 30%. A key feature of the Checklist’s design was covering all the essentials without requiring the input of resources or equipment that may not be available to surgical teams.
One necessary exception to the equipment rule appears in item four on the Checklist: “Is the pulse oximeter on the patient and functioning?”
Pulse oximeters measure oxygen saturation in the blood, commonly using a noninvasive sensor that clamps lightly onto the finger. They alert medical professionals if a patient’s blood oxygen levels dip below a safe threshold, and have been part of the standard of care in surgery with general anesthesia for decades. And yet, as of a decade ago, they were absent from an estimated 77,000 operating rooms worldwide, according to the nonprofit Lifebox Foundation.
Lifebox, founded in 2011 by the Association of Anaesthetists of Great Britain and Ireland, the World Federation of Societies of Anaesthesiologists, the Brigham and Women’s Hospital, and the Harvard T.H. Chan School of Public Health, made it its mission to get reliable pulse oximeters into resource-limited surgical contexts. Putting pulse oximeters in the hands of surgical teams that would otherwise be without them would raze one major hurdle to the Checklist reaching its full lifesaving potential.
Not just any pulse oximeter would serve, though, since unreliable equipment can be worse than no equipment at all. Lifebox sourced a device—the eponymous “Lifebox”—with rechargeable batteries to weather power interruptions, a sturdy construction to survive rough use without need for maintenance, an intuitive-to-use design, and a price affordable enough to distribute it at scale.
More important than the technology, though, are the networks of medical professionals who use pulse oximeters, adopt the Surgical Safety Checklist, and collectively determine the culture of operating rooms. Lifebox follows locally specific partnership models, collaborating with organizations and individuals on the ground to distribute the device, and engages hospital staff in direct trainings and “Training of Trainer” workshops.
Credit: Lifebox
Two grants from the Stavros Niarchos Foundation (SNF) supported Lifebox from 2016 to 2019 in expanding its organizational capacity and in carrying its work related to the pulse oximeter and safe anesthesia into India.
In the year of Lifebox’s inception, 2011, nearly half of operating rooms in India did not have access to pulse oximeters. With support from SNF, the organization has donated 748 pulse oximeters to healthcare facilities, provided training to more than 1,000 healthcare professionals across nine Indian states, and trained nearly 50 trainers on the ground.
At trainings, participants discussed the WHO Surgical Safety Checklist and safe surgery practices, learned how to use the Lifebox pulse oximeter, walked through case studies for its use, and developed action plans for when anesthesia goes wrong.
Lifebox estimates that the donated pulse oximeters have helped contribute to the safety of more than 700,000 surgeries each year in India, and the oximeters operate almost universally for a minimum of five years.
In January, Lifebox and Ariadne Labs issued a “Checking in on the Checklist at 10 Years” report on where things stand and where we need to go from here. As noted in the New York Times coverage of the report, the Checklist is employed in 90% of surgeries in wealthy countries, but only one third of those in poorer countries.
The report identified a number of factors contributing to this disparity, and Lifebox continues to work for safer surgical outcomes on a number of different fronts, building on steadily expanding reach and leveraging its increased capacity. It continues to forge new partnerships with anesthesia societies and other medical professionals around the world. Its “Clean Cut” program seeks to reduce surgical infection, and it’s pushing forward on a project to develop a headlamp that will help address the inadequate surgical lighting conditions affecting an estimated 24 million patients each year.
All told, Lifebox has so far donated more than 20,000 pulse oximeters to surgical teams in over 100 countries.
If this multipronged, multi-continent effort sounds terribly complex, rest assured that the organization appreciates the value of taking things step by step.
Learn more:
-Read the “Checking in on the Checklist at 10 Years” report and the New York Times piece covering it
-Read Dr. Atul Gawande’s 2009 book The Checklist Manifesto: How to Get Things Right
-Download the Surgical Safety Checklist app, and never be caught without your checklist when you have to perform surgery

Source: Vainateya Gavai

Source: Vainateya Gavai
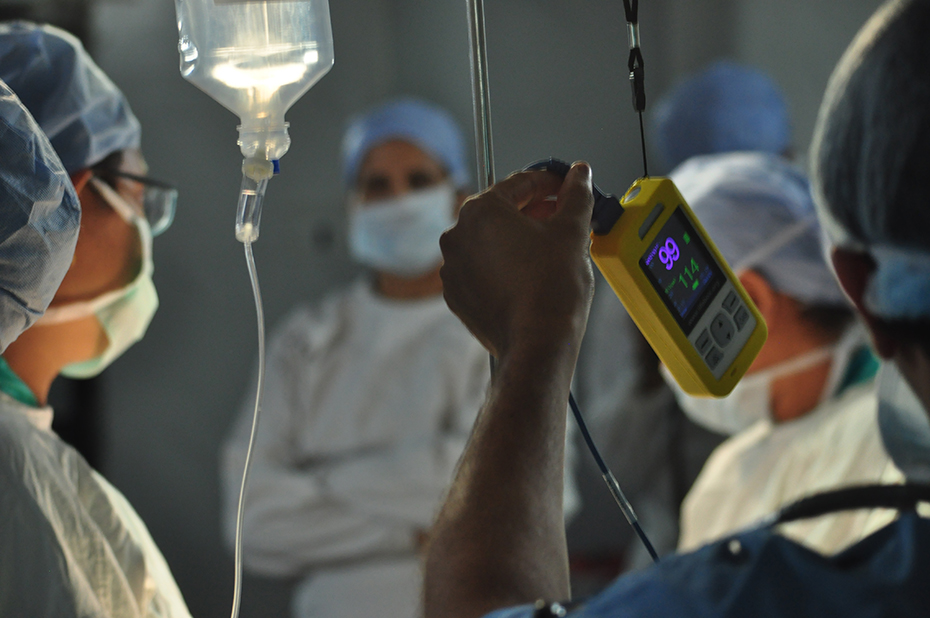
Source: Vainateya Gavai
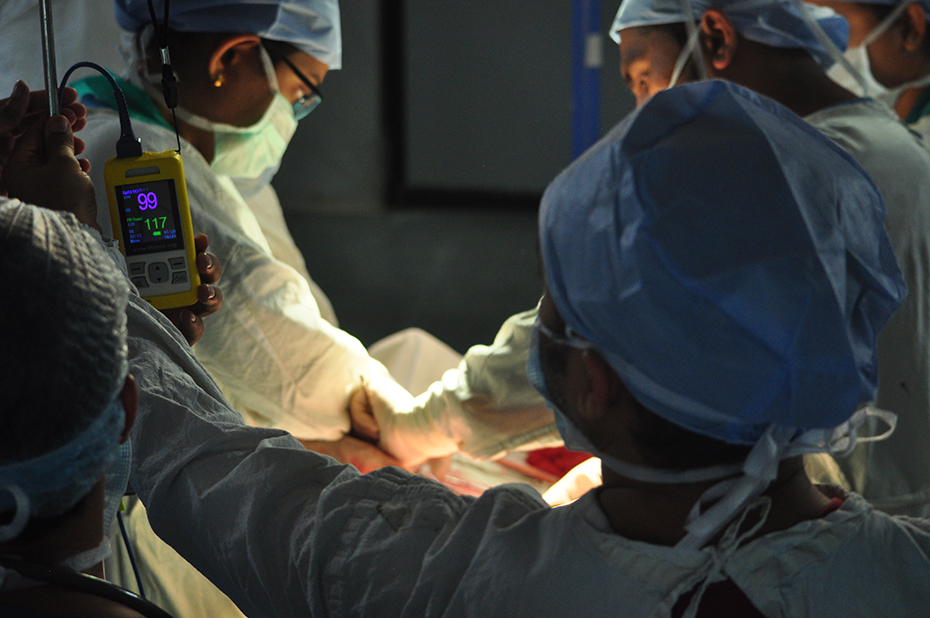
Source: Vainateya Gavai
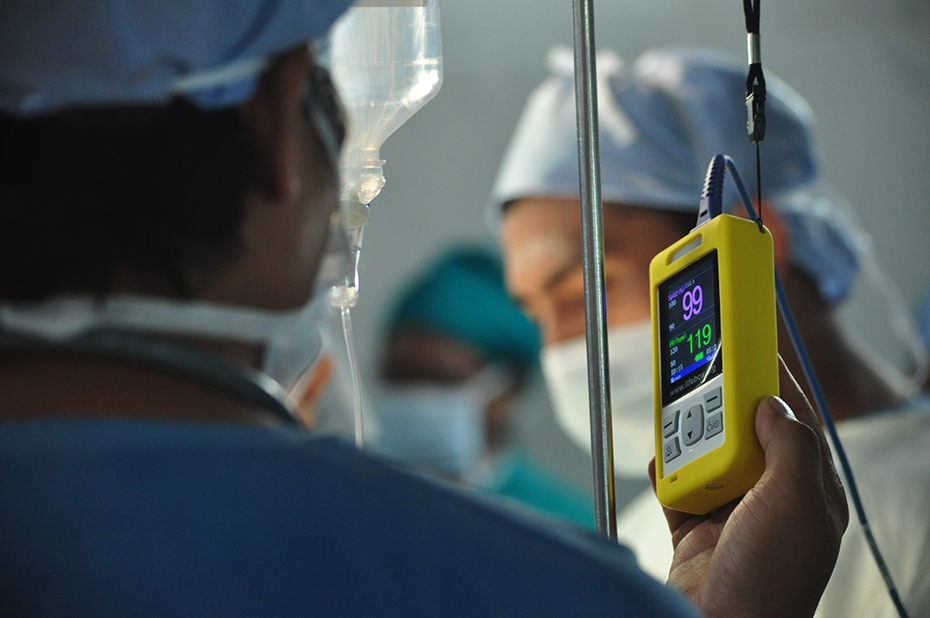
Source: Vainateya Gavai
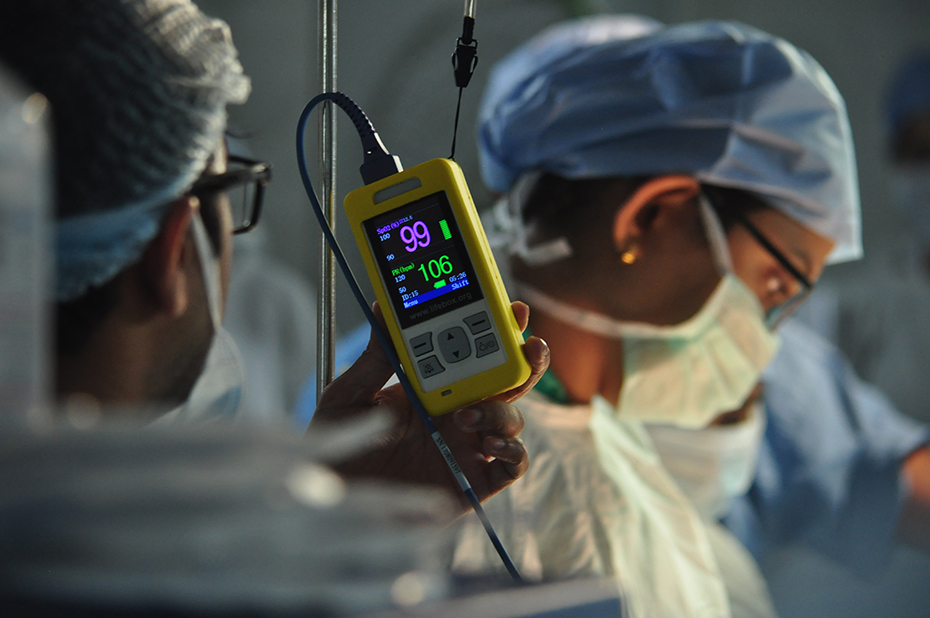
Source: Vainateya Gavai
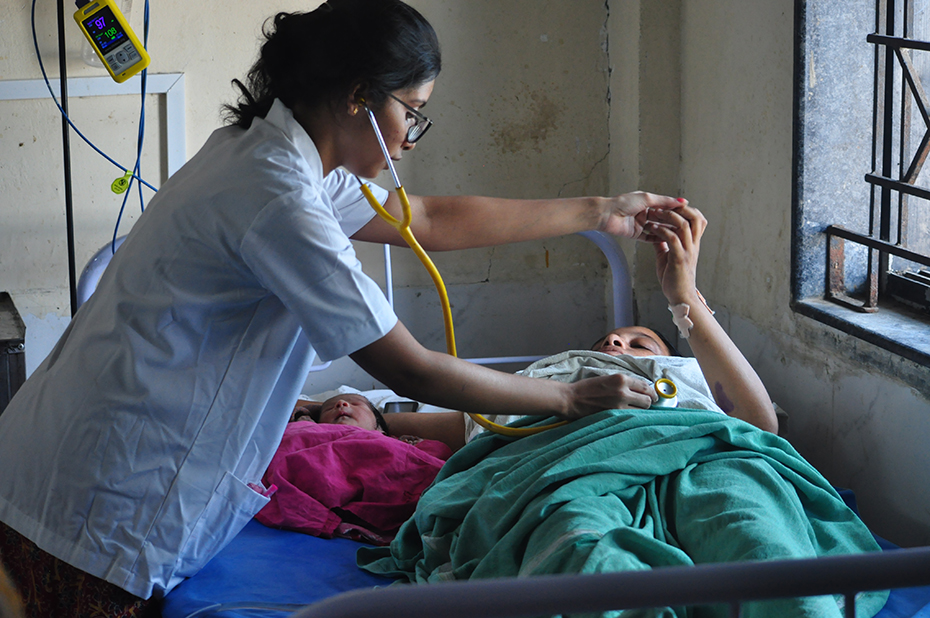
Source: Vainateya Gavai

Source: Ritesh Uttamchandani

Source: Ritesh Uttamchandani
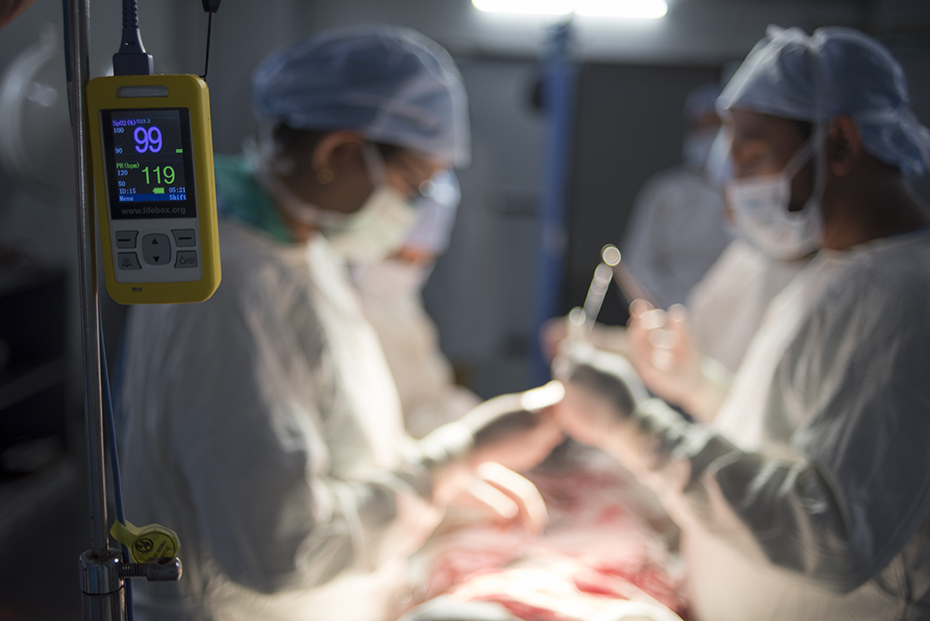
Source: Ritesh Uttamchandani
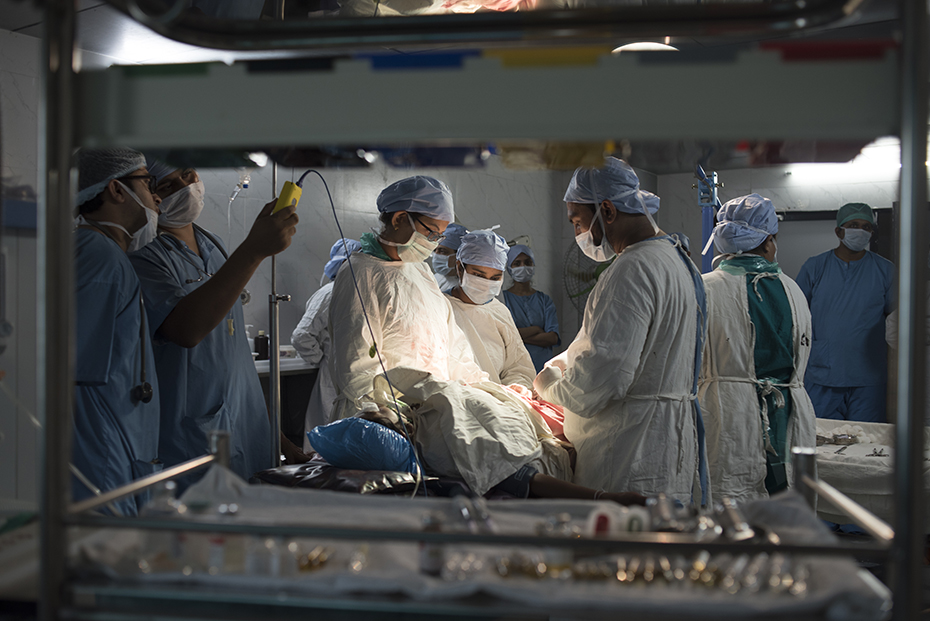
Source: Ritesh Uttamchandani